Answer
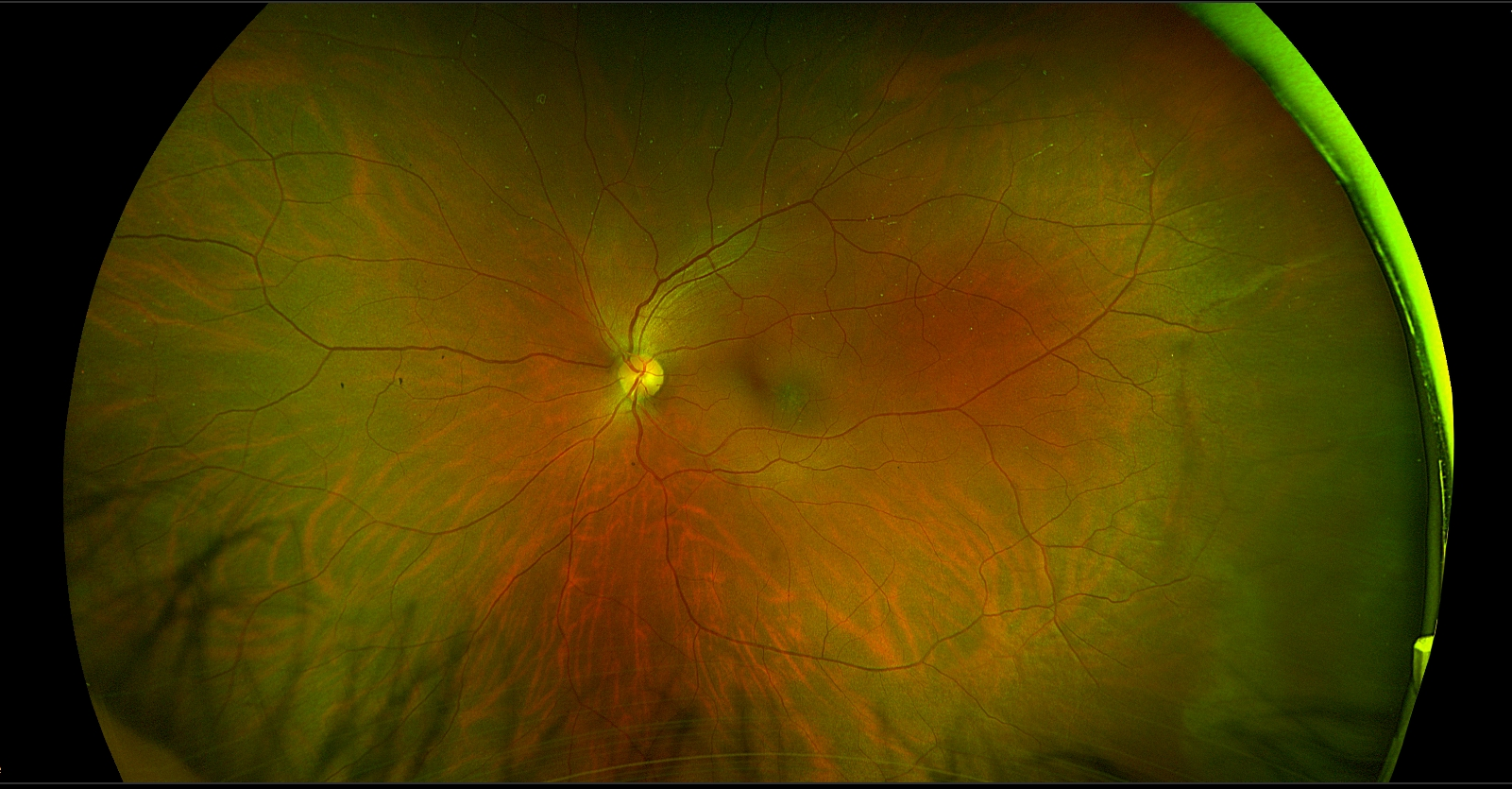
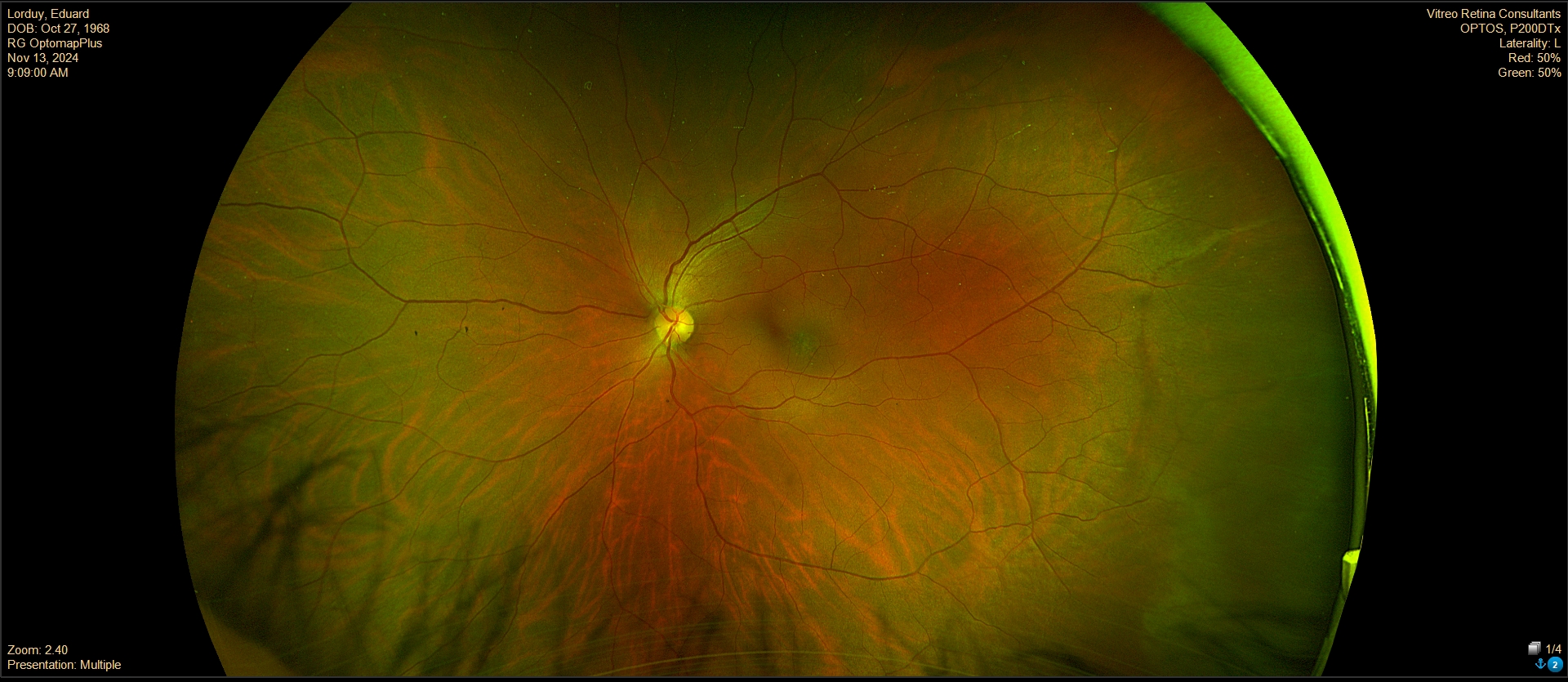
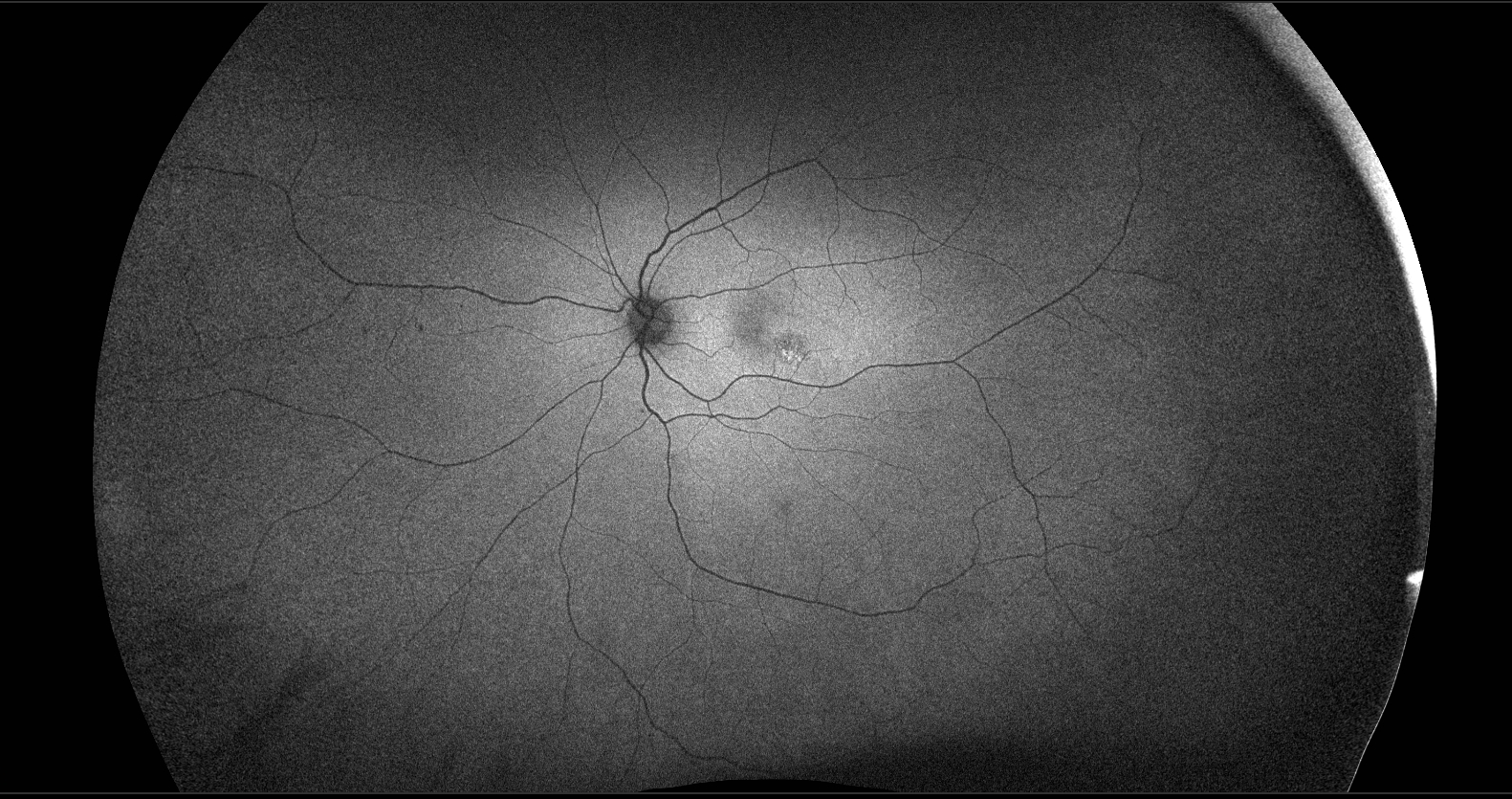
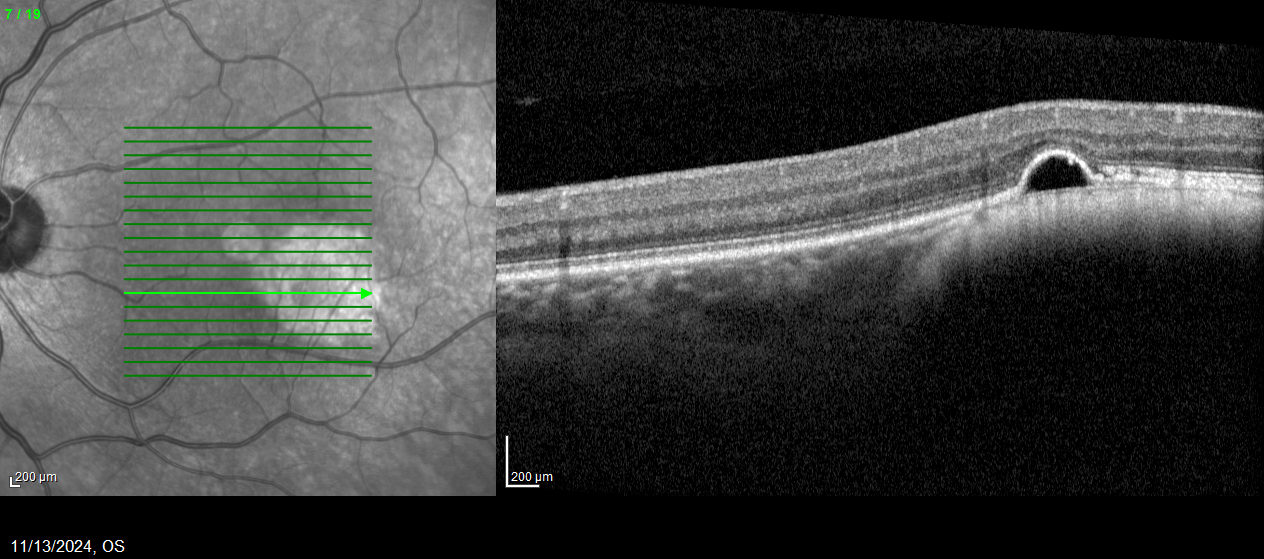
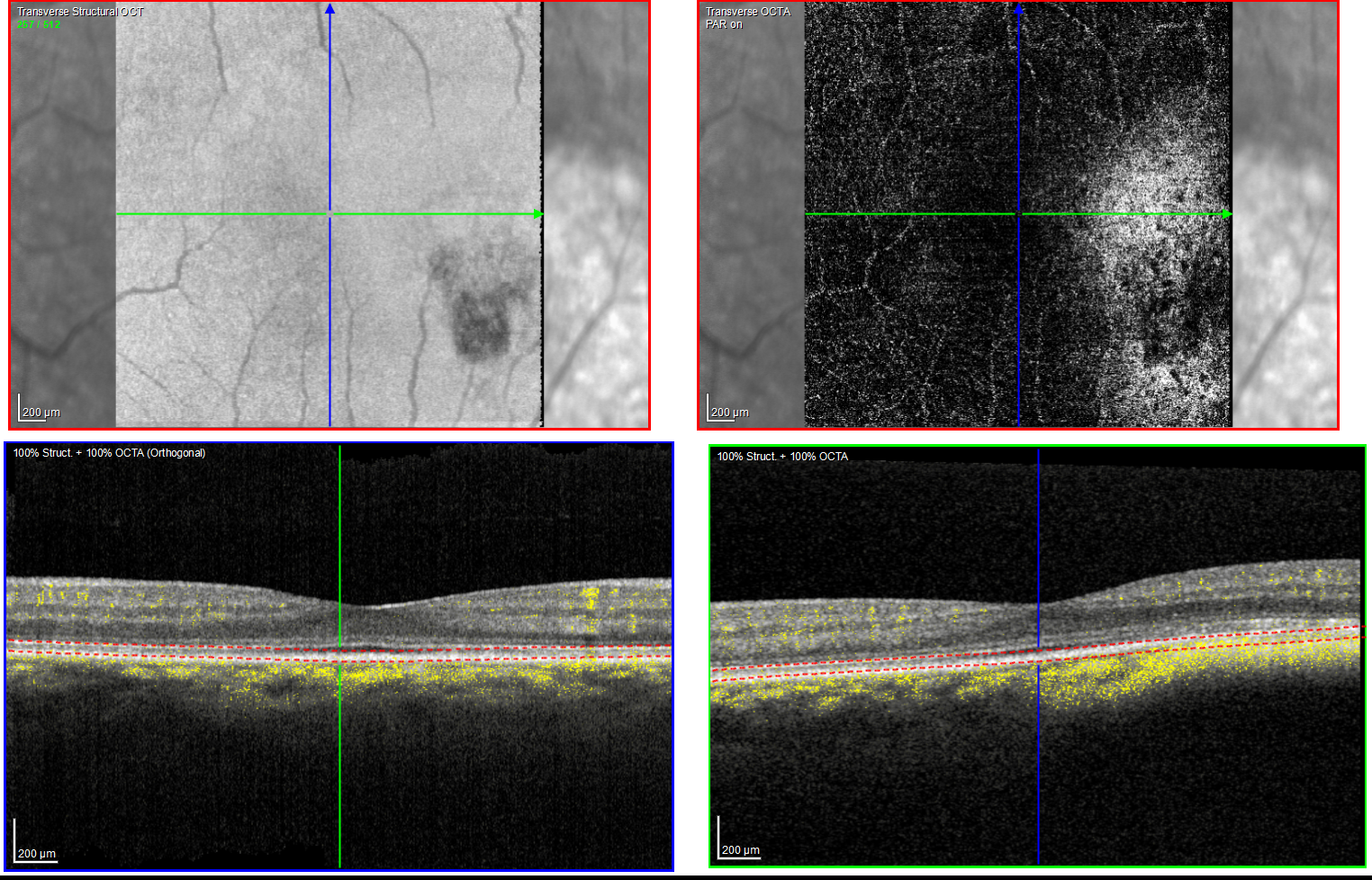
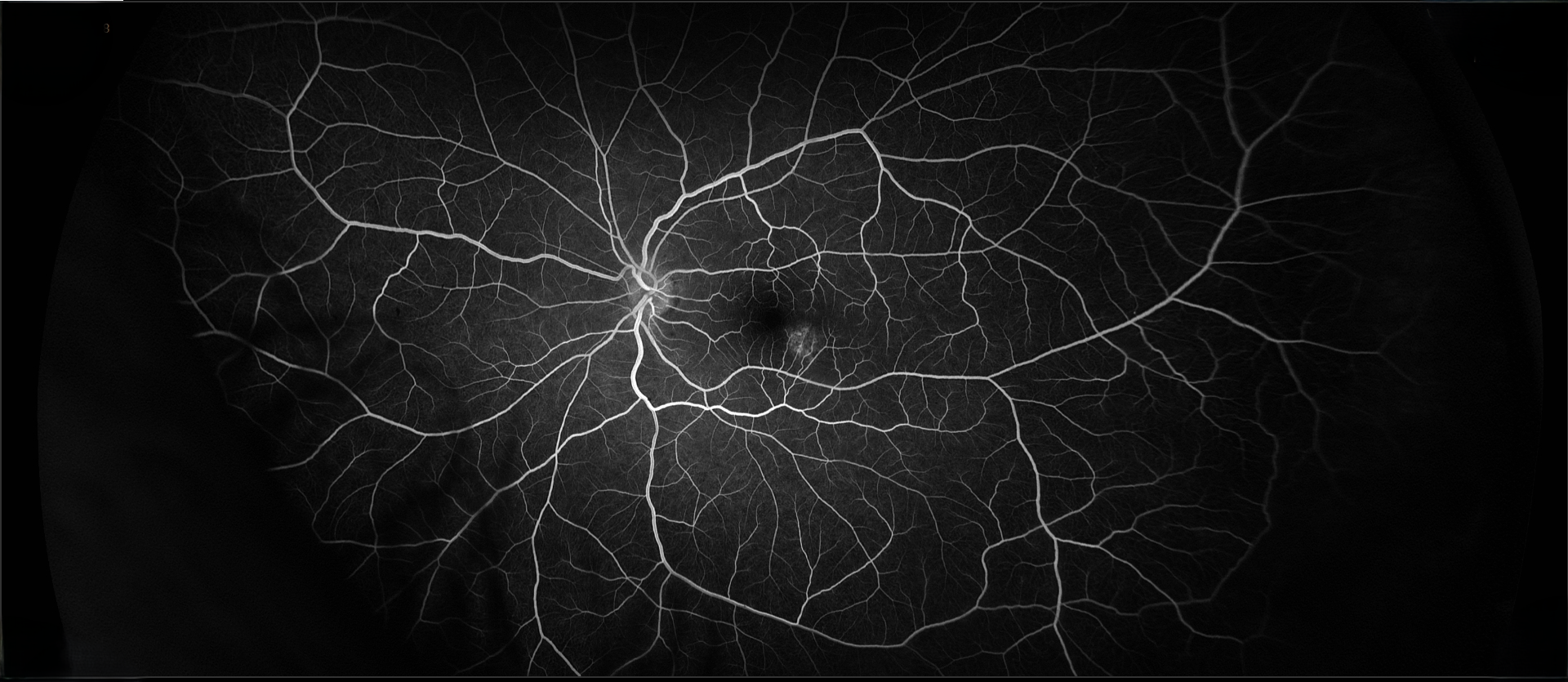
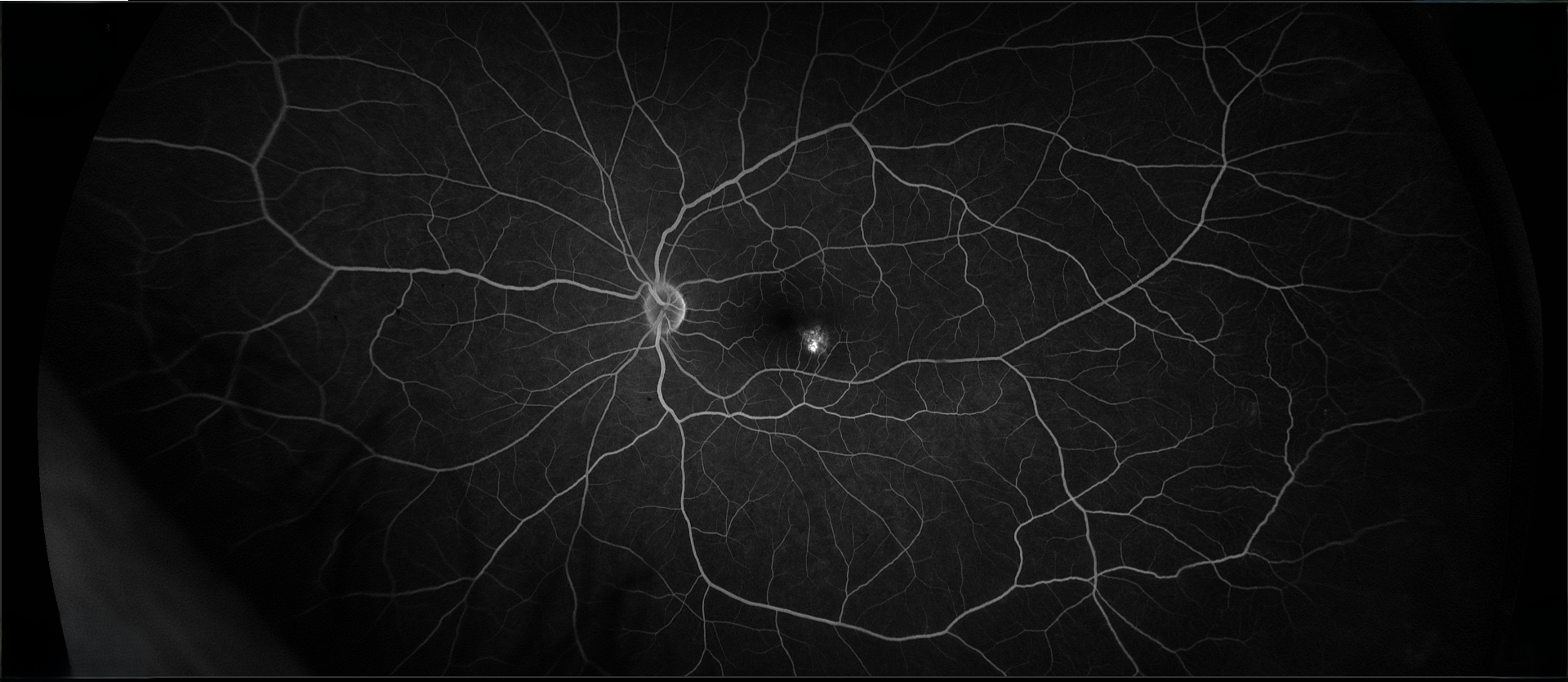
The patient had a small, flat pigmented lesion in the left macula. Fundus autofluorescence showed punctate hyperautofluorescence. Optical coherence tomography (OCT) demonstrated a minimally elevated choroidal mass that had replaced the normal choroidal vasculature. There was a serous pigment epithelial detachment without subretinal fluid or macular edema. OCT angiography did not reveal a choroidal neovascular membrane (CNVM). Fluorescein angiography showed mottled hyperfluorescence in both early and late phases without evidence of leakage.
These findings are most consistent with a choroidal nevus associated with a pigment epithelial detachment. Although CNVMs can arise over nevi, no evidence of CNVM activity was detected in this case. An occult CNVM remains a possibility, and the patient is being monitored accordingly. The punctate hyperautofluorescence raises the possibility of a small melanoma, and the presence of overlying subretinal fluid increases this concern. However, there has been no change in the size or characteristics of the lesion over the past year.
Pigment epithelial detachments associated with nevi, in the absence of CNVM activity, have been reported but are very uncommon.
Shabto JM, Wells JR, Grossniklaus HE, Azarcon CP. Case series: Retinal pigment epithelial detachments over choroidal nevi – what is the clinical significance? Ocul Oncol Pathol 2025;11:125-131.